6 Things To Know If You’re Immunocompromised And Considering A 3rd Shot
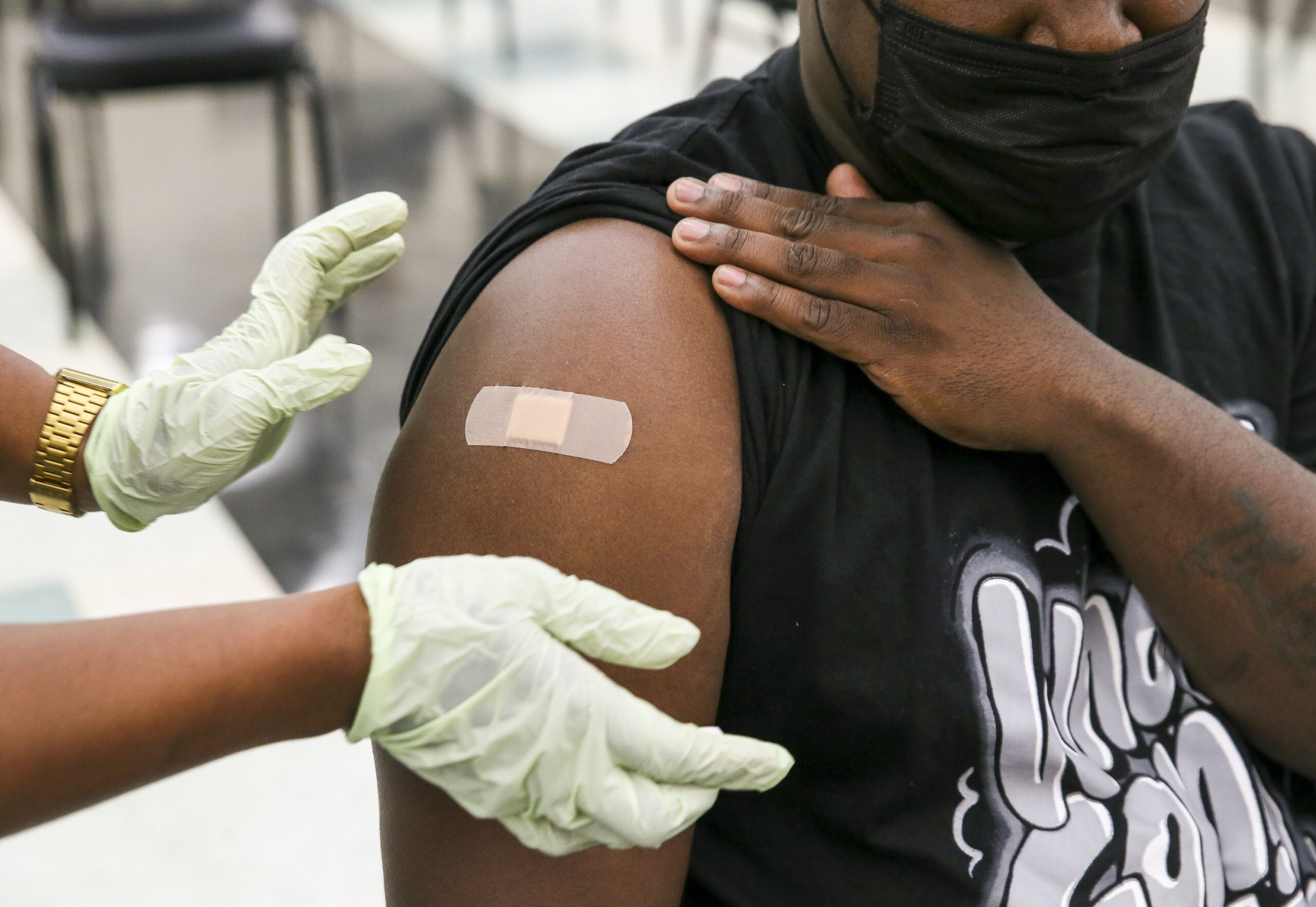
Dorchester – August 5: A Covid-19 vaccine is administered at the Harvard Street Neighborhood Health Center vaccine site at Prince Hall Grand Lodge in Dorchester, MA on August 5, 2021. (Photo by Christiana Botic for The Boston Globe via Getty Images)
Christiana Botic / Boston Globe via Getty Images
People with compromised immune systems who already got two doses of the Pfizer or Moderna vaccines can now get a third shot to boost their protection from COVID-19.
This week’s decision by federal health agencies is welcome news to many patients and their doctors who have been calling for this for months.
“I’m really excited,” says Pat Beale, 59, of Boise, Idaho, who lives with a liver transplant and takes medicine that suppresses his immune system. He plans to get his third dose within the next week.
Data show that many immunocompromised patients, such as organ transplant recipients and others on immune-suppressing medications, have had weak responses to the initial doses of the vaccine.
For Dr. Marc Boom, who runs Houston Methodist Hospital, the authorization for third shots couldn’t have come soon enough for patients in his hospital’s large transplant program.
“We are immediately pulling in those people, getting them the doses,” Boom says. He applauds the FDA’s decision, but says the agency could have acted faster, noting that countries like Israel, France and the U.K. have already made this move.
Friday’s recommendations from the Centers for Disease Control and Prevention leave some questions about exactly who is eligible for an additional dose and how to get it. Here’s what we know so far.
1. Why should immunocompromised people get a third shot?
Having a compromised immune system puts you at higher risk of severe illness and death from COVID-19. Studies show that the initial vaccine doses are less effective for people with weakened immune systems, ranging from 59% to 72%, compared to 90% to 94% among people without serious immune deficiencies.
People with conditions that weaken the immune system are also far more likely to have a breakthrough infection than people in more normal health. One U.S. study shows 40% to 44% of hospitalized breakthrough cases are in immunocompromised people.
“If I was someone who was on one of the medications that was on the CDC list, you know, I would almost consider myself unvaccinated at this point,” says Dr. David Karp, who heads the Division of Rheumatic Diseases at UT Southwestern Medical Center.
Karp says that even though the current delta surge has mostly hit unvaccinated people, vaccinated but immunosuppressed patients are also landing in hospitals with COVID-19.
“For this group of patients, you know, a third shot is going to improve their response to the vaccine and therefore lessen their chances of either contracting the disease or having a more serious disease,” says Karp, who is also president of the American College of Rheumatology.
For patients like Valen Keefer, who is a liver and kidney transplant recipient in California, knowing there’s a way to get a third shot is a relief.
“This is an amazing and such an important step and needed for a while for our transplant community,” she says. “It’s just been so hard to know what to do and when to do it.”
2. Who should get third shots?
Only a very small group of people with weakened immune systems qualify for the third dose. The CDC is recommending it for moderately to severely immunocompromised people, including those who have:
- Been receiving active cancer treatment for tumors or cancers of the blood
- Received an organ transplant and are taking medicine to suppress the immune system
- Received a stem cell transplant within the last two years or are taking medicine to suppress the immune system
- Moderate or severe primary immunodeficiency (such as DiGeorge syndrome, Wiskott-Aldrich syndrome)
- Advanced or untreated HIV infection
- Active treatment with high-dose corticosteroids or other drugs that may suppress your immune response
The recommendation is limited to adults 18 and older for the Moderna vaccine because that vaccine has not been authorized for adolescents as of yet. The Pfizer vaccine is authorized for adolescents 12 and older, and adults.
3. I don’t know if I’m immunocompromised but I do have a chronic disease that makes me vulnerable to severe COVID-19 — should I be getting a third shot?
Many people may consider themselves at higher risk of serious illness from COVID-19 due to age or a pre-existing condition, and may want another dose of vaccine. But, for now, an additional shot is only recommended for people who meet the CDC’s criteria for being immunocompromised.
People with other chronic conditions — even those that put them at higher risk for severe COVID-19 — are not authorized to get an additional dose at this point.
“This would not include long-term care facility residents, persons with diabetes, persons with heart disease — those types of chronic medical conditions are not the intent here,” said Dr. Amanda Cohn at Friday’s CDC committee meeting.
It’s not clear yet whether or when a booster will be recommended more broadly to vulnerable populations, though this is already underway in other countries including Israel. Health officials are currently tracking how well immunity holds up in people enrolled in the vaccine clinical trials. Those trials will determine timing of booster shots, officials of both the FDA and CDC say.
4. Can I just sign up to get the shot or should I talk to my doctor first? And do I have to prove I’m immunosuppressed?
Start by talking with the health care provider you see for your immune-suppressing condition or its treatment. A doctor’s note is not likely to be required at vaccine sites — a person just needs to inform the staff that they are moderately to severely immunocompromised. However, it’s best to get your doctor’s input before getting the shot, says Dr. Dorry Segev, a transplant surgeon and researcher at Johns Hopkins University who has been studying COVID-19 vaccination among organ transplant recipients.
He says that your doctor can help you determine if the benefits of getting a third shot outweigh any risks in your particular case. “My hope is that this will be an individual patient-provider shared decision,” he says.
For people with compromised immune systems, “every time we activate the immune system, there is a risk,” Segev cautions. For instance, transplant recipients could risk rejection of the organ. “These things need to be done in a very careful, deliberate, thoughtful way with people’s medical teams,” he says.
For patients with certain conditions, it may be necessary to pause their immune-suppressing medications temporarily to let the third dose of the vaccine take effect, explains Karp. So talk to your doctor about your situation and how to increase your chances of having the vaccine be effective.
5. If I get a third shot, how good is the protection?
There are many different reasons people can be immunosuppressed — it’s often a combination of their age, their medical conditions, what treatments and drugs they’re taking. While studies show that a third vaccine dose can boost antibody responses in some people, it’s not universally guaranteed to work.
Immunocompromised people who get a third shot should still be aware they’re not necessarily safe from COVID-19, warned Dr. Helen Keipp Talbot during the ACIP committee meeting.
“I think the reality is they’ll be safer, but still at an incredibly high risk for severe disease and death.” And everyone they spend time with also needs to be vaccinated, to protect them, Talbot says.
In a presentation to the committee, the CDC’s Dr. Kathleen Dooling said immunocompromised people, including those who receive an additional dose, should continue to follow prevention measures, including wearing a mask, staying six feet apart from others they don’t live with and avoiding crowds and poorly ventilated indoor spaces. And she also urged close contacts of immunocompromised people to get vaccinated if they’re not already.
6. Do I need to get the same vaccine I got for my first two doses? And what do I do if I got the J&J vaccine?
The CDC recommends you get the same vaccine you got for your first two doses, so if you got the Pfizer or Moderna the first two doses, get that one for your third shot. But if that is not feasible, the CDC committee said an additional dose with the other mRNA vaccine is permitted.
Currently only the Pfizer and the Moderna vaccines are authorized for an additional dose. If you got the J&J, you still aren’t eligible.
The FDA says that there wasn’t enough data available to extend the authorization for an additional dose for the J&J shots. Representatives of both the FDA and the CDC said that they are “actively engaged” to determine the best course of action for recipients of the Johnson & Johnson vaccine and expect to know more “very shortly.”
9(MDAxODM0MDY4MDEyMTY4NDA3MzI3YjkzMw004))





