Street Medicine Brings Health Care To Atlanta’s Homeless
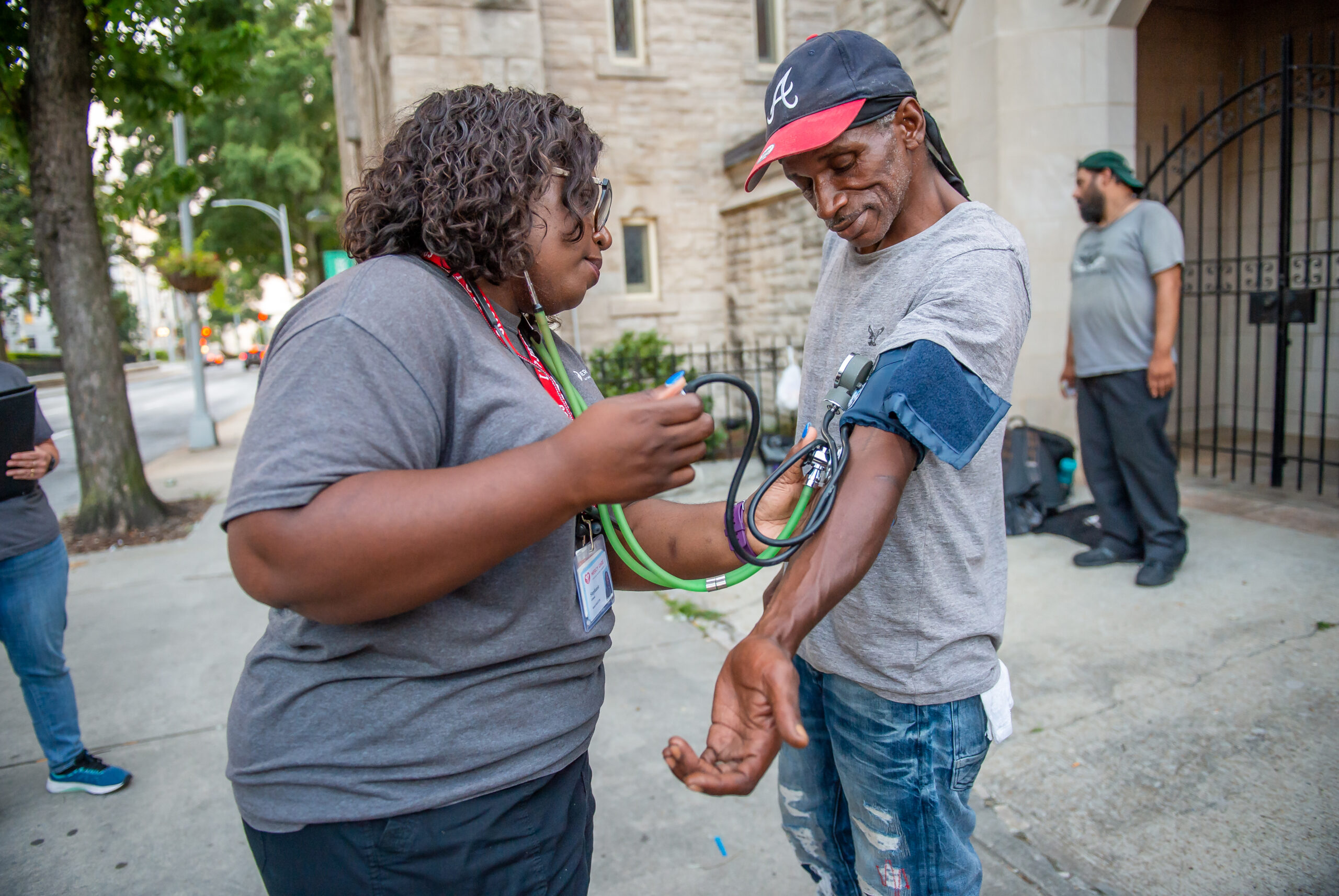
Licensed practical nurse Stephanie Dotson measures the blood pressure of Kent Beasley outside Central Presbyterian Church in downtown Atlanta on Sept. 9. Dotson is a member of the Mercy Care Street Medicine team, which works to provide medical and behavioral health care to the city’s homeless population.
Bita Honarvar / For WABE
It’s late afternoon, and a large van sits idling in the hot sun on a street corner in southwest Atlanta near where Interstate-20 crosses over Whitehall Street.
Herman Ware sits surrounded by medical supplies at a wobbly table in the vehicle. He’s taking a break from the mid-September heat, as nurse Stephanie Dotson prepares to give him a flu shot.
“Well it might sting, yeah, I figured that,” Ware says in anticipation.
Ware has been living under the interstate for a few months now. The Army veteran says he’s doing alright, save for the occasional aches and pains.
His big problem these days? Mosquitoes. So, Dotson gives him some insect repellent as she sends him on his way.
“Take care! I got that flu shot out the way,” Dotson calls after Ware as he steps off the bus.
Interactions like these can be rare for people experiencing homelessness. For those trying to find a hot meal or a place to sleep, health can take a backseat.
That’s where street medicine programs come in, such as the one run by Mercy Care since 2013. Four days a week, the clinic sends medical teams to spots in the city where homeless people gather to offer a range of services.

Gaining Trust
Nurse practitioner Joy Fernandez de Narayan has been doing this work, off and on, for about five years. She stands outside the van greeting patients as MARTA trains pass on tracks nearby.
“When we’re coming out here to talk to people, we’re on their turf,” she said.
That means she can never assume people want her help, whether that’s a vaccination or a snack
“We’ll sit down next to someone, like ‘How’s the weather treating you?’ And then kind of work our way into: ‘You mentioned you had a history of high blood pressure. Do you mind if we check your blood pressure?’” de Narayan said.
She says it can take several encounters to gain someone’s trust and get them into care.
The medical team also has to get creative with the remedies they prescribe, because simple things can be hard to come by.
“Such simple things,” de Narayan said. ‘“You go to the doctor, because you have a sore throat, and they’re like, ‘Gargle warm salt water.’ Well, out here, it’s like, ‘Ok, well where am I going to get water?’”
But those limitations don’t stop the street medicine team from helping people.
Sopain Lawson has been living in this spot under I-20 for most of the summer. That’s where she developed a foot fungus that sidelined her for an entire month.
“I couldn’t walk. I needed help. I had to stay off my feet,” Lawson said. “And the crew, they took good care of my foot. They got me back.”
Lawson attributes her recovery to weekly visits from the street medicine team. She’s friendly with the practitioners and hugs de Narayan before walking off.
“This is what street medicine is about: going out into these areas where people are not going to seek attention until it’s an emergency,” said Matthew Reed, a social worker with the group. “We’re trying to avoid emergencies, but we’re also trying to build relationships.”
As a freight train rolls by, Reed says those relationships are crucial. They help the street medicine team convince people to seek out other services: mental health counseling, dentistry, even housing.
‘Go To The People’
There are dozens of similar programs around the country, according to the Street Medicine Institute.
Dr. Jim Withers is medical director of the group. He started making house calls to the homeless in 1992 with Pittsburgh Mercy’s Operation Safety Net. Mercy Care is part of the same Catholic parent organization, Trinity Health.
“Health care likes people to come to it on its terms,” Withers said. “The philosophical central point of street medicine is: go to the people.”
Doing that work in Atlanta costs Mercy Care about $900,000 a year. The clinic estimates its street medicine helped at least 300 people connect to care in 2018.
These programs are important, Withers says, because the health care system isn’t reaching people who are homeless.
“There’s all these populations: they’re still sick, they’re still coming to the emergency rooms, and we’re not dealing with them well,” he said. “They stay in the hospital longer. They have more complications.”

And that care costs a lot of money. One recent estimate says Atlanta’s homeless population racks up more than $60 million in emergency room visits and hospital stays.
“The sickest patients require the most time and effort. That’s true regardless of whether the person is housed or homeless,” said Dr. Stephen Hwang, who studies homelessness and health at St. Michael’s Hospital in Toronto.
Hwang says it’s not clear if street medicine has a large-scale impact. Instead, he says each personal interaction can add up.
“Every encounter that they have on the street with someone is actually, in and of itself, an indicator of effectiveness,” he said.
It’s twilight as the Mercy Care team pulls up to its final stop of the night, Central Presbyterian Church in downtown Atlanta.
A handful of people settle down for the night on the sidewalk as traffic whizzes by on Washington Street.
Among them is Johnny Dunson, a frequent street medicine patient who talks with members of the street medicine team like they’re old friends.
“You gotta’ let someone know how you’re feeling, understand me? It’s a lot of people that need some kind of assistance to do what you’re supposed to be doing, and they do a wonderful job,” he said.
Dunson says the Mercy Care team gives him the help he needs, and they do it with respect. Living out here, it can be hard to find either.









