It’s Not Just Measles. What You Should Know About Vaccines For Adults
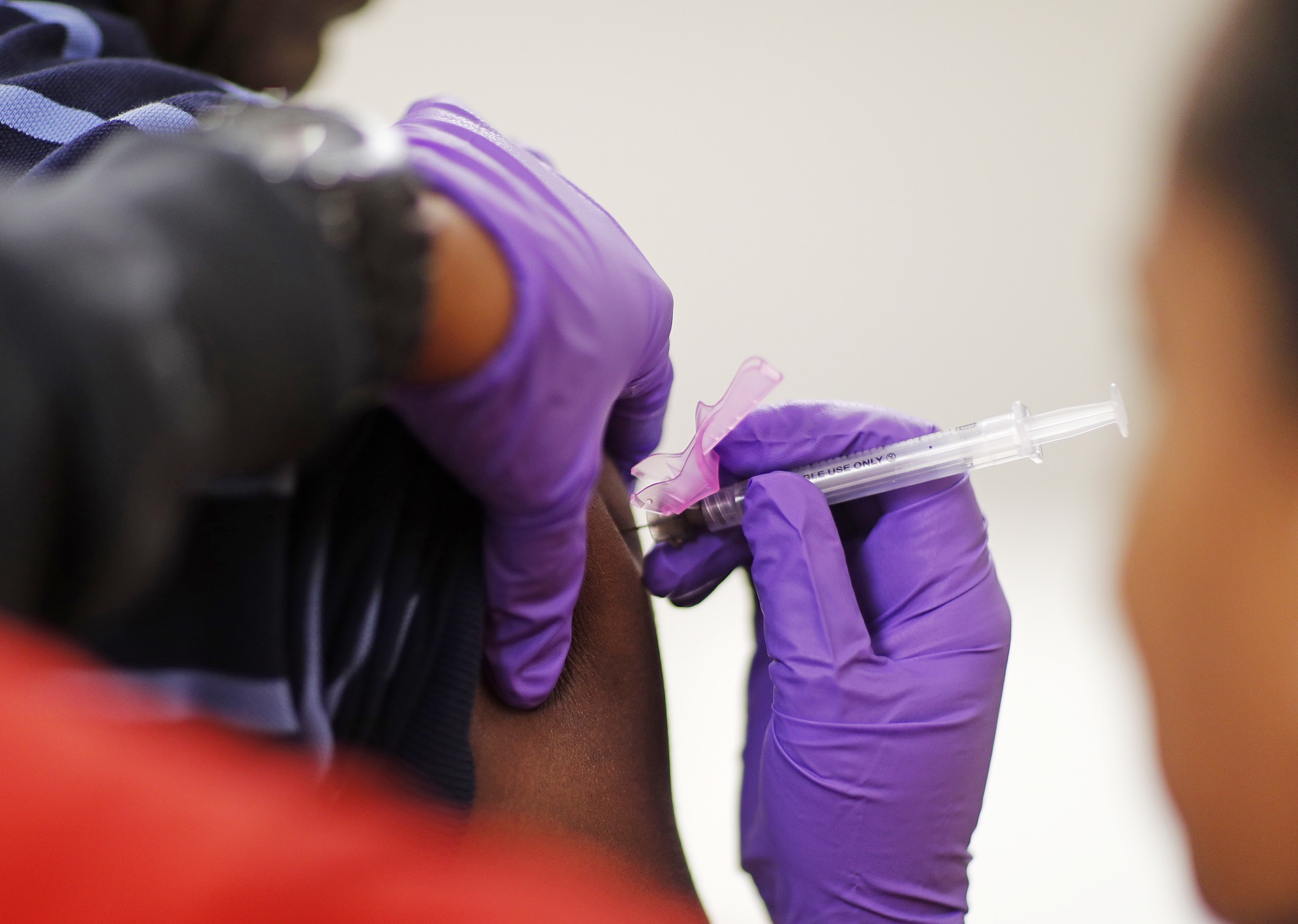
Many people might not be aware of what types of vaccines they need as they get older.
David Goldman / Associated Press
Updated at 1 p.m. ET
Amid one of the largest measles outbreaks in the U.S. in recent history, vaccines are on the minds of many Americans.
The Centers for Disease Control and Prevention reported this week that the number of measles cases this year has climbed to 839 in 23 states, affecting mostly unvaccinated people. Most people in the U.S. are vaccinated against measles when they’re children as part of the routine immunizations they get in primary care.
We’re used to kids needing lots of shots to ward off lots of illnesses, but what about adults? The CDC recommends that adults get multiple vaccines for conditions ranging from tetanus to influenza to cervical cancer. The shots can be a bit trickier to keep track of, as many adults go to the doctor less frequently than kids do, but those vaccinations are equally important for staying healthy.
“Many adults are not aware of what vaccines they actually need,” says Dr. Pamela Rockwell, an associate professor of family medicine at the University of Michigan who works with the CDC’s Advisory Committee on Immunization Practices. “That is also balanced by physician unawareness of what vaccines they should be recommending. It’s gotten very complicated, and it is difficult to keep up with all the changes.”
So we’re here to answer some common questions about adult vaccines. Click on each topic to go to that section.
1. Measles 2. Shingles 3. Tetanus 4. Vaccines during pregnancy 5. Before meeting a newborn baby 6. Before visiting the elderly 7. Chickenpox 8. Hepatitis B, A and C 9. HPV
I was vaccinated against measles as a child, but the measles outbreak makes me worry that I’m no longer immune. Do I need to be revaccinated as an adult?
If you received the standard two doses of the modern measles, mumps and rubella (MMR) vaccine, you’re all set. You shouldn’t need to be revaccinated, because you’re considered immune for life.
And if you were born before 1957, doctors assume you were exposed to measles as a child and are already immune.
However, a version of the vaccine produced in the mid-to-late 1960s wasn’t as effective as the current regimen, so if you were vaccinated before 1968, you should talk to your doctor about whether you need another shot. If you were born after 1957 but for some reason never got immunized, you should also get the MMR vaccine.
I’ve heard there’s an effective vaccine for shingles, but my doctor’s office doesn’t have it and it’s out of stock at the pharmacy. What’s going on?
Shingrix is a two-dose vaccine that is upward of 95 percent effective at preventing shingles, a painful rash that tends to affect older adults and immunocompromised people. The vaccine was approved in 2017 and requires two injections. It’s more effective than Zostavax, an older shingles vaccine, so doctors will recommend Shingrix over Zostavax to most patients over age 50.
There has been a shortage of Shingrix for almost as long as it has been available because demand for the vaccine has outpaced the supply. Its manufacturer, GlaxoSmithKline, told the CDC that it’s working to step up its production schedule. But because every dose of Shingrix needs to undergo safety checks, GSK expects that shortages will continue at least through the end of the year.
“The demand was so great they literally couldn’t keep up,” Rockwell says.
If you get the first dose, do your best to get the second one within two to six months. If your local pharmacies don’t have Shingrix in stock, don’t worry — you can use the HealthMap Vaccine Finder to find out where it is available. If you wait more than six months to get the second dose, you don’t need to repeat the first one, but it’s possible the vaccine won’t be quite as effective in preventing shingles.
What’s the deal with tetanus shots? How often do I need them?
Tetanus is a life-threatening disease of the nervous system that’s caused by a toxin-producing bacterium usually found in soil. It can be prevented by a series of five childhood shots, including a booster between ages 11 and 12. Adults then need a booster shot every 10 years. It can be hard to keep track of this if you move or change doctors, so make a note in your calendar and don’t be afraid to ask about it. If you get it early or a year or two late, it isn’t harmful.
If you ever have an injury that might expose you to tetanus — such as stepping on a nail — your doctor will ask when your latest tetanus booster was and may give you another booster shot on the spot. If you’re not up to date on your tetanus vaccines, you may need additional treatment to prevent the disease.
Childhood tetanus shots are combined with a vaccine for diphtheria, a dangerous infection that can affect kids, and one for pertussis, which is known as whooping cough. Your every-10-year tetanus and diphtheria boosters won’t include pertussis, unless you’re pregnant. But when you turn 65, you should again get the shot that protects against all three, which is known as Tdap.
I’m thinking about having a baby. What vaccines do I need?
Make sure you and everyone around you is up to date on standard childhood and adolescent vaccines, including pertussis, since babies are vulnerable to this disease. You should also get a dose of Tdap during prenatal care, since it’s safe in pregnancy.
Everyone also should get an annual flu shot, because pregnant women, who have weakened immune systems, are particularly susceptible to influenza and can get very sick or die from an infection.
Even if you got all the recommended vaccines as a kid, it’s possible your immunity has waned when it comes to some of the vaccine-preventable diseases that can be passed from mom to baby. This is why prenatal doctors and midwives check to make sure pregnant women are immune to hepatitis B, varicella (chickenpox) and rubella.
If you find out you’re not immune before you get pregnant, you should get vaccinated again. The hepatitis B vaccine is safe during pregnancy. But the varicella and MMR (which includes rubella protection) vaccines are not safe for pregnant patients, so your doctor is likely to recommend that you get them after delivery.
I’m planning to visit my newborn nephew. What vaccines do I need?
If you’ve gotten all your recommended vaccines and boosters, you’re almost ready to meet the baby. Babies, like pregnant women, have weak immune systems, so an annual flu shot is important before interacting with a newborn. Adults over 65 should have gotten a pertussis booster (included in the Tdap shot).
What about if I’m visiting my hospitalized, elderly grandmother?
Older, hospitalized adults are similar to newborns in that their immune systems are weak and particularly vulnerable to infections. Follow the same advice as if you’re going to meet a new baby.
I was born before the varicella (chickenpox) vaccine existed. Do I need it now?
The varicella vaccine was approved in 1995, so if you were born before then, there’s a good chance you weren’t vaccinated.
But even if you weren’t vaccinated, you’re probably already immune because there’s a high likelihood you’ve had chickenpox. The CDC says adults born before 1980 don’t need the vaccine and don’t need testing to prove their immunity.
There are some occasions when doctors will want to order blood tests to make sure their patients are actually immune to varicella — for pregnant women and health care workers, for example. If you get tested and the blood test shows you’re still susceptible, your doctor will recommend that you get the vaccine. But because the vaccine is so effective and the blood test isn’t always accurate, getting tested isn’t necessary for everyone.
What do I need to know about all the different hepatitis shots?
Hepatitis means inflammation of the liver, but when we’re talking about vaccines, we’re referring to several types of viruses that infect liver cells and can cause lots of different and potentially life-threatening problems, ranging from diarrhea to liver failure to cancer. Routine childhood immunizations include vaccines for hepatitis A and hepatitis B, meaning virtually all kids in the U.S. are vaccinated against them.
Hepatitis B is transmitted through blood or sex. A vaccine for it has been available since the 1980s, but it’s common for immunity to hepatitis B to decrease over time. If you work in health care or are thinking about becoming pregnant, your doctor might order a blood test that shows if you’re still immune. If you’re not, your doctor may recommend you get revaccinated as an adult.
Hepatitis A is transmitted through the fecal-oral route, meaning that if you eat something that has been contaminated with the feces of an infected person, you can get it. The vaccine for hepatitis A was approved in 1995. If you’re not yet vaccinated and you fall into one of a few groups — including if you’re a man who has sex with other men, you’re traveling to a country where the virus is endemic, you live with a person who has had hepatitis A — you should get the shots.
Hepatitis C is another common viral infection that affects the liver. It’s so common, in fact, that doctors routinely test people born between 1945 and 1965 for the virus. Unfortunately, there’s no vaccine available for it, but it can be treated with an oral medication. If you haven’t been screened for it, ask your doctor if you need to be.
Who should get the HPV vaccine? What’s it for?
This is essentially a cancer vaccine.
The Food and Drug Administration initially approved the HPV vaccine for girls and young women in the early 2000s, but the range of people who should get it has since grown. The FDA recently approved its use for people up to age 45. FDA approval is different from CDC guidelines, however. The CDC still officially recommends that both boys and girls get their first shot by 11 or 12, up until age 26 for women and 21 for men. The CDC adds that men up to age 26 “may be vaccinated” based on a consult with a doctor. If you’re older than 26 and haven’t been vaccinated, again, talk to your doctor about whether you need it.
HPV stands for the human papillomaviruses, which cause a wide variety of conditions, ranging from common warts on hands and feet to cervical and anal cancer. The vaccine helps prevent infection from certain types of HPV, including the strains that are the most likely to cause cancer.
It’s a series of two shots, six to 12 months apart, which is a change from when the vaccine was first approved — it used to require three shots. Children who are late getting the HPV vaccine and receive their first dose after age 15 will still need three doses.
And there’s more.
You may also need vaccines for conditions such as pneumonia or meningitis. Ask your doctor. What your doctor recommends will depend on your medical history and your risk factors, so don’t be afraid to speak up at your next appointment. You can use this CDC quiz to see what might be right for you.
Mara Gordon is a family physician in Washington, D.C., and a health and media fellow at NPR and Georgetown University School of Medicine.
9(MDAxODM0MDY4MDEyMTY4NDA3MzI3YjkzMw004))