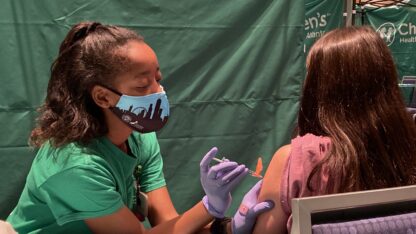
Pandemic Pushing Medicaid Numbers Higher As Many Lose Work
States that have expanded their Medicaid programs under the Affordable Care Act (ACA) are expected to have even bigger increases in enrollees, because they allow more coverage for low-income adults.
U.S. Centers for Medicare and Medicaid Service via AP
Georgia data indicate that the economic crisis caused by the pandemic has begun to have an effect on enrollment in Medicaid and the Children’s Health Insurance Program.
As COVID-19 ravaged the state over the past two months, new Medicaid and PeachCare enrollment in Georgia has increased 38%, versus the same period of time in 2019.
There were also smaller increases in January and February. But over March and April, the state programs saw 88,000 new enrollees, as compared with 64,000 in those months last year.
Enrollment in Medicaid typically increases during an economic downturn. When people lose their jobs, they often lose health insurance coverage for themselves and their families. That leads to children and some adults being enrolled in safety-net programs.
About 2 million Georgians are currently members of Medicaid and PeachCare – and most of them are children.
States that have expanded their Medicaid programs under the Affordable Care Act (ACA) are expected to have even bigger increases in enrollees, because they allow more coverage for low-income adults.
At the same time, with all the job losses, Georgia is likely to see a big jump in the number of people who are uninsured, says Bill Custer, a health insurance expert at Georgia State University.
Georgia already has the third-highest rate of people without health insurance, at 13.7%.
“We could easily get back to 20% or over that we had before the ACA,’’ Custer says. “Most people think we’re in for a fairly long recession.’’
One option for people losing coverage is COBRA, a federal program that continues coverage for some terminated workers, but that can be very expensive. People losing job-based coverage can also try to get special enrollment coverage through the ACA insurance exchange for one or more family members.
In March, Insurance Commissioner John King directed all health insurers in the state to refrain from canceling health policies for the cause of non-payment until further notice.
That directive expires at the end of May.
King, in an April 28 bulletin, added that he ‘‘encourages health insurers to be accommodating towards consumers who find themselves in financial difficulty.’’
Letting the non-cancellation directive lapse would be premature, said Laura Colbert of the consumer group Georgians for a Healthy Future.
“Many Georgia consumers are still going to be out of work at the end of May, and if they are back at work, many will be catching up on rent, utilities, and credit card bills,’’ Colbert said Thursday. “Georgians will struggle to make up premium payments at the same time.”
State leaders, she said, “should prioritize actions that preserve and expand the number of Georgians with health insurance.”
People without health insurance are more likely to skip needed medical care due to costs. That often leads to more serious health problems.
Overall, the impact of these coverage shifts on the health care system could be profound. “In the financing of the health care system, we really haven’t yet felt the effects of this in health care in Georgia,” Custer says.