The CDC Said The Delta Variant Is As Contagious As Chickenpox. That’s Not Accurate
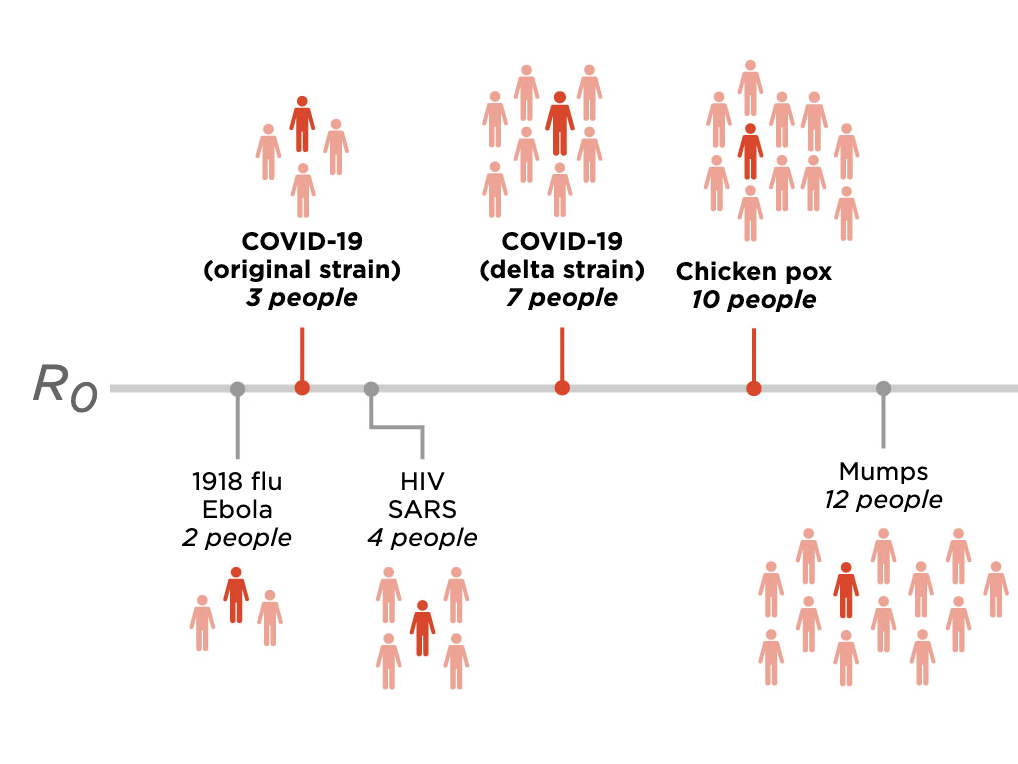
The number of people that one sick person will infect (on average) is called R0. Here are the maximum R0 values for a few viruses.
In a leaked report, the Centers for Disease Control and Prevention made a surprising claim about the delta variant of the coronavirus: It “is as transmissible as: – Chicken Pox,” the agency wrote in a slideshow presentation leaked to The Washington Post on July 26.
Chickenpox is one of the most contagious viruses known. Each individual can spread the virus to as many as “90% of the people close to that person,” the CDC reports.
Is the delta variant that contagious as well?
The short answer is no, says evolutionary biologist and biostatistician Tom Wenseleers at the University of Leuven in Belgium.
“Yeah, I didn’t find the CDC’s statement entirely accurate,” says Wenseleers, who was one of the first scientists to formally calculate the transmission advantage of the alpha and delta variants over the original versions of SARS-CoV-2.
Nonetheless, delta is still highly transmissible, he adds. “It’s probably the most contagious respiratory virus that we know, for the moment,” he says.
Here’s why.
When scientists measure a virus’s transmissibility, they often use what’s known as R0, or “R nought. ” It’s the number of people a sick person will infect when the entire population is vulnerable to the virus.
“So it’s the virus’s potential of spreading, given ideal conditions for the virus, when no one has any immunity,” says computational biologist Karthik Gangavarapu at the Scripps Research Institute.
For example, the flu has an R0 of about two. Each person infected with flu passes the virus on to two people on average. Some people will infect more than two people, and some will infect fewer. But over time, the average will be about two.
Chickenpox, on the other hand, is way more contagious, Gangavarapu says. Chickenpox has an R0 of about nine or 10. So each person with chickenpox infects about 10 other people on average. Outbreaks are explosive.
For SARS-CoV-2, the R0 has actually risen over the course of the pandemic as the virus evolved. When the coronavirus first emerged in 2019, SARS-CoV-2 was slightly more contagious than flu, Gangavarapu says. “The initial COVID-19 strain had an R0 between two and three.”
Then about a year later, the virus began to mutate quickly. The alpha variant emerged, likely in the U.K., and was more transmissible than the original strain. A few months later, the delta variant emerged, most likely in India. It was even more transmissible than alpha.
“For the delta variant, the R0 is now calculated at between six and seven,” Wenseleers says. So it’s two- to three-times as contagious as the original version of SARS-CoV-2 (R0 = 2 to 3) but less contagious than the chickenpox (R0 = 9 to 10).
So why did the CDC say the delta variant was “just as transmissible as” the chickenpox?
For one, the leaked document underestimated the R0 for chickenpox and overestimated the R0 for the delta variant. “The R0 values for delta were preliminary and calculated from data taken from a rather small sample size,” a federal official told NPR. The value for the chickenpox (and other R0s in the slideshow) came from a graphic from The New York Times, which wasn’t completely accurate.
“At the end of the day, this delta variant is much more transmissible than the alpha variant,” the official added. “That’s the message people need to take from this.” The official requested anonymity because they were not authorized to speak to the media on this topic.
The difference between an R0 of three and six is massive. For example, with the original strain of SARS-CoV-2, one person would infect about three people, and each of those people would infect three more. So after only two rounds of transmission, cases would rise by nine (3 x 3 = 9). After three rounds, cases would rise by 27 (3 x 3 x 3 = 27). But with the delta variant, the first person would infect six others, who would each then infect six more people. So after two rounds of transmission, cases would already rise by 36 (6 x 6 = 36). After three rounds, cases would surge by 216 (6 x 6 x 6 = 216).
With an R0 of six, delta will be extremely difficult to slow down unless populations reach high levels of vaccination, Wenseleers says. And even then surges in cases will still occur, as is now happening in Iceland and parts of the U.S. The vaccine is less than 90% effective at stopping infections with delta, and vaccinated people can still spread the virus. In addition, people who aren’t vaccinated have a very high risk of infection, Wenseleers says. “Anyone that chooses not to get vaccinated will in all likelihood get infected by the delta variant over the coming months.”
For example, in San Francisco, daily case levels are rapidly rising toward those seen last winter despite the fact that more than 70% of the population is vaccinated, per San Francisco Department of Public Health reports.
Although cases of delta are inevitable, hospitalizations aren’t, Wenseleers points out. “As long as people would get vaccinated, then we will not get huge wave of hospitalizations.” For example, the city of San Francisco has had 3,041 people hospitalized with COVID-19 since March 18, 2020. Only 16 of them were fully vaccinated.
9(MDAxODM0MDY4MDEyMTY4NDA3MzI3YjkzMw004))








