Amid Rural Hospital Crisis, One Georgia Hospital Thrives

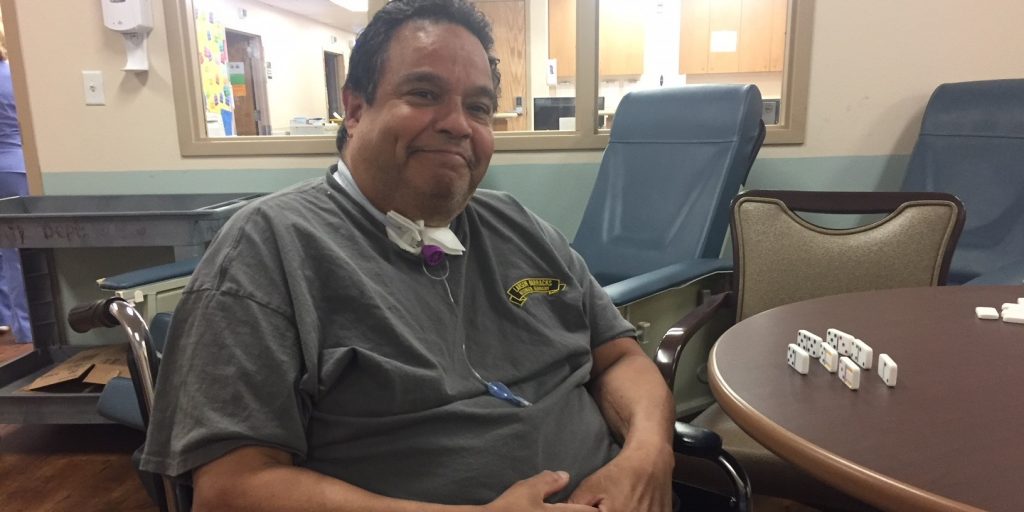
Miller County Hospital in Colquitt, Georgia, has been able to survive by creating a niche service — ventilator care in its nursing home.
Elly Yu / WABE
Two years ago, David Roman Reyes was hanging out in his apartment in Fort Myers, Florida, when he started feeling sick.
“I was just doing normal stuff in the house, and I was getting ready to go to bed, and all of a sudden I had a tremendous feeling of chills — uncontrollable.”
Reyes called his neighbors, who then called an ambulance. The next thing he knew, he woke up three days later in a hospital, with a tracheal tube in his neck.
“I was down for three days, so I didn’t really know what was going on,” Reyes said.
Reyes, 62, said he later learned he suffered septic shock, and had to have three blood transfusions. He’s been in recovery ever since and uses a ventilator to help him breathe at night. That’s why he’s been at Miller County Nursing Home in Colquitt, Georgia, about three and a half hours south of Atlanta, over the past year.
“It’s been a journey,” he said.
Born and raised in New York, Reyes jokes he’s still getting used to Colquitt.
“I’m a city guy, you know, so everything here’s like country,” he said. “And, you know, they try their best to convert you into a country boy, but I’m not going for that yet.”
‘A Tremendous Gamble’
Reyes is one of about 60 patients at Miller County Nursing Home that needs ventilator care. The nursing home is part of Miller County Hospital. The ventilator program wasn’t always part of the facility, but it’s one way the hospital has been able to keep its doors open, said Robin Rau, Miller County Hospital’s CEO.
“It was a tremendous gamble that we took, but it was either that, or we were going to close,” she said.
When Rau became the hospital’s CEO about a decade ago, she said the hospital, like many other rural hospitals, was in bad shape. It was $6 million dollars in debt, and its nursing home had about 30 empty beds, she said. And then, the recession hit.
“I thought for sure it would be a minor miracle if this place stayed open,” she said.
Rau said the facility needed patients – so she looked towards Atlanta, including Grady Hospital, where there was a much larger population of patients in need. But beyond that, she said she recognized the need to develop a specialty, or niche, in nursing home care.
“They had a tremendous amount of uninsured people, homeless people, people with disabilities who didn’t have home, didn’t have access,” she said.
The nursing home transferred patients who needed specialized care for trach tubes to Miller County. Then, its social workers helped the patients get insurance, like Medicaid for people with disabilities, so that the nursing home could get paid for services. The hospital spent millions investing in specialized equipment and staff, and the nursing home began specializing in a ventilator care program, Rau said.
Rau acknowledges all of this was a big risk.
“They were uninsured. We didn’t have money but we had a vision and we thought we could help everybody out and develop a relationship and help those individuals and ultimately help ourselves,” she said.
‘Manna From Heaven’
It paid off.
After eating the costs for about nine months, she said the hospital started getting reimbursements from the government.
“All of a sudden, it was like manna from heaven,” Rau said.
Besides finding this niche in ventilator care, Rau found other ways to make ends meet. The hospital opened a pharmacy, which allowed the hospital to save money by filling prescriptions in-house. It gave free doctor visits to employees of local companies to attract those with insurance. And it started to cut down unnecessary emergency room visits by offering more services at a rural clinic and managing people’s health, Rau said.
“I’m trying to keep people healthy so they’re not in our emergency room,” Rau said. “It costs me maybe $100, $110 to see somebody in our rural health clinic – that’s my cost. But if they come into my emergency room, it’s going to cost me a lot more than that.”
All these efforts have saved the hospital. Today, Rau said the hospital authority employs about 500 people in a county with just under 6,000 people. This during a time when many of the state’s rural hospitals are losing money. At least six rural hospitals have closed in Georgia since 2012.
“For survival, that recipe is you’ve got to have vision, you’ve got to have good leadership, you’ve got to have a willingness to diversify,” said Jimmy Lewis, CEO of Hometown Health, an organization that represents rural hospitals in Georgia.
He praises Miller County’s success but said it’s an anomaly. He said there are forces outside of a rural hospital that can make it hard for them to survive, like serving a sicker population, more uninsured people, and receiving fewer payments from the government.
“For this to be replicated across the rest of the state, you never say never, but it would be extremely difficult,” Lewis said.
But for Miller County Hospital, Rau said they’re looking at what’s next. Construction is ongoing next to the hospital to add space for 50 more nursing home beds.