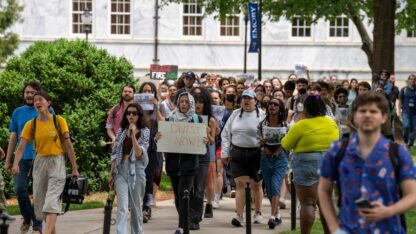Diagnostic Gaps: Skin Comes In Many Shades And So Do Rashes
But rashes, just as one example, are problems for people of all colors, and they don’t always look red on dark skin. They can look kind of purple or may barely show up at all. And when doctors haven’t seen examples on darker skin, they may not be able to give an accurate diagnosis.
Kristen Uroda for NPR
When Ellen Buchanan Weiss’ son was about a year old, he broke out in a rash — little bumps that appeared to be hives. So Buchanan Weiss did what a lot of new parents do: She turned to the internet to find images that matched the rash she was seeing on her little boy.
“I’m trying to figure out — would I be paranoid if I went to the doctor at this point? Is that a reasonable thing to do? So I started Googling it,” says Buchanan Weiss, who lives with her family in Raleigh, N.CG
But her son has brown skin, and as she scrolled through the photos that came up, she couldn’t find any images of rashes that matched her little boy’s — there were none on people of color. Even when she looked at the usually reliable webpages of the Centers for Disease Control and Prevention, for example, or the Mayo Clinic’s, she faced the same problem.
“It became immediately clear to me,” she says, “that the vast majority of even common skin conditions are on white skin. You have to scroll down like 80 pictures to find a single one on brown skin.”
Lynn McKinley-Grant, a dermatology professor at Howard University and president of the Skin of Color Society, says that’s not just a problem with websites aimed at patients.
“Often in medical schools,” she says, “they have limited pictures of diseases in skin of people of color.” That means health professionals trained with these resources aren’t seeing the full picture, McKinley-Grant says. The diversity gap is embedded in medical training, and that should concern us all.
Medical school classes rely on a lot of pattern recognition — especially when it comes to dermatology, explains Art Papier, an associate professor of dermatology at the University of Rochester Medical Center, in New York. “You see picture after picture, to encode them into your brain,” he says.
“You take these residents — they look at thousands of cases. And you’re training them to see the skin, classify what they see.”
In 2006, Papier and his colleague, Dr. Tobechi Ebede, published an analysis of major textbooks and other educational and training resources in dermatology and found photographs of darker skin to be sparse. Until recently, Papier says, “examples in people of color were limited to diseases that were more common in people of color.”
But rashes, just as one example, are problems for people of all colors, and they don’t always look red on dark skin. They can look kind of purple or may barely show up at all. And when doctors haven’t seen examples on darker skin, they may not be able to give an accurate diagnosis.
As a practicing dermatologist, McKinley-Grant has seen this firsthand. “I’ve had patients who have said they go in and they tell the doctor that they have redness. And the doctor can’t see it. They’re like, ‘Well, there’s nothing there. Just put some lotion on and go home.’ ”
McKinley-Grant says schools are now making an effort to diversify training materials. But they’ve still got quite a ways to go.
And this problem could get even worse. Roxana Daneshjou is a dermatology resident at Stanford University. For her doctorate work, she’s looking at the use of artificial intelligence in medical diagnosis.
“If we don’t fix the biases we have in health care before we jump to training a computer to do it, we’re just going to actually perpetuate those biases,” explains Daneshjou.
The computer learns the same way students do — Daneshjou and her team feed it image after image to create a tool that can help it, and doctors, recognize patterns. And when there aren’t images of darker skin in its database, the algorithm — like a doctor — won’t be as good at diagnosing people of color. That’s true whether the origin of the skin problem is an allergic reaction, Lyme disease or cancer.
“So addressing bias and improving diversity are not tangential issues,” stresses Daneshjou. “They’re actually central to providing equitable health care.”
This lack of diversity in training tools is a problem that people are still struggling with at the very foundation of medical training. LaShyra Nolen, a first-year student at Harvard Medical School, says the issue came up last month in her microbiology class when she and her classmates were shown an image of the classic Lyme disease bull’s-eye rash.
When someone asked how the disease presents on darker skin, the professor struggled to provide an answer, Nolen says.
Traditionally, the standard of medicine — in everything from classroom images to CPR dummies — has been white and male, she says, “and that is just not going to cut it anymore. We have to move and shift and change in the same direction as our population. If not, we’re going to be unable to provide our diverse patient population with the best care that they deserve.”
So how do you get more diverse images? Specialized resources aimed specifically at doctors and medical students — including a visual diagnostic guide edited by McKinley-Grant — are moving into the mainstream curriculum.
But people have to seek them out. And they may not even realize what’s missing.
Buchanan Weiss, who couldn’t find pictures that looked like her son two years ago, has since created a resource she hopes will be part of the solution — the answer was right on her phone.
She launched the Instagram account Brown Skin Matters in August, posting photos of various skin conditions on people of color. In just a few months, she has accumulated more than 7,000 followers.
“I expected moms to want this resource,” acknowledges Buchanan Weiss. “But I’ve been surprised by how much of the attention has been from medical professionals.”
All the dermatologists we spoke with stressed that no Instagram account or database should substitute for a medical exam. But it is a resource, they say. And it’s helping raise awareness of the problem. Which is one of the first steps to making sure that the picture of future medicine looks a little different — and more realistic.
9(MDAxODM0MDY4MDEyMTY4NDA3MzI3YjkzMw004))