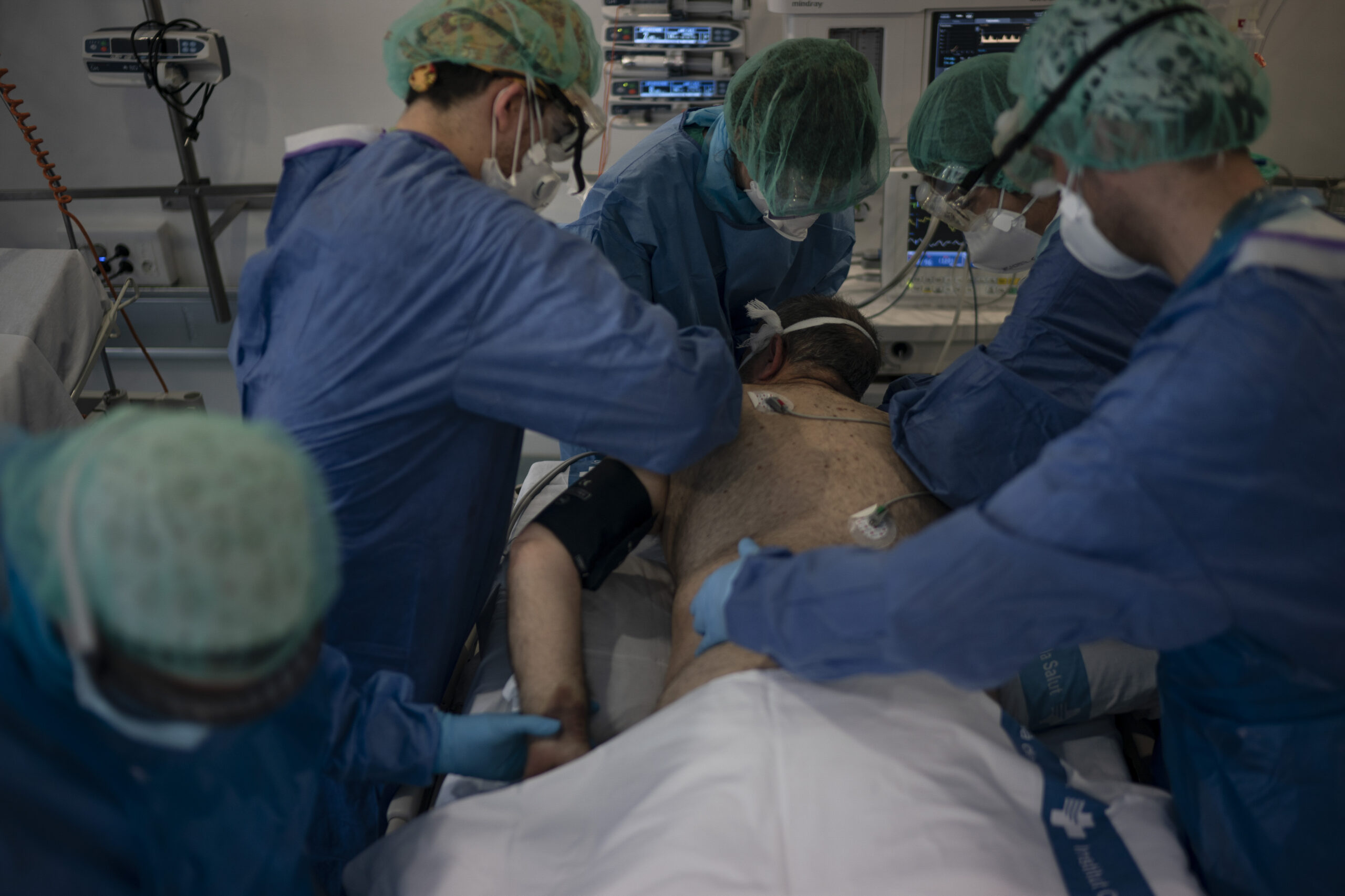
When patients on ventilators aren’t getting enough oxygen into their bloodstreams, one thing doctors will try is flipping them over onto their stomachs.
Prone ventilation has been in use for patients with Acute Respiratory Distress Syndrome, or ARDS, for years, but now hospitals are trying something new with COVID-19 patients; having them lie prone before they have to go on a ventilator.
Having COVID patients on ventilators lie on their stomachs was already a clear choice, said Dr. Craig Coopersmith, interim director of the Emory Critical Care Center.
Read this story now for free
To continue reading, sign up for our newsletter and get unlimited access to WABE.org
You can select your preferences for news and local content. We will never share your email address. Learn how your newsletter sign-up will support WABE and Public Media