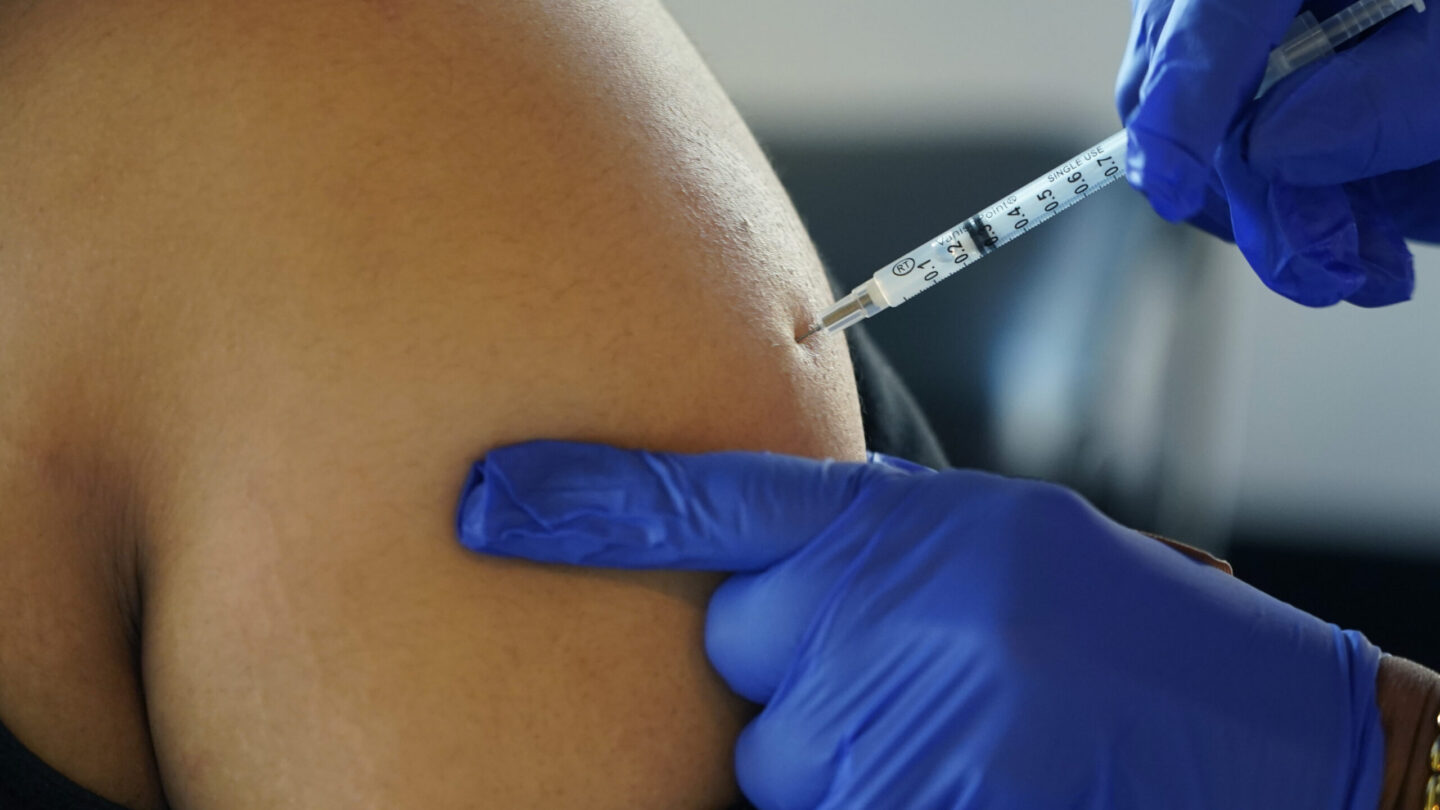
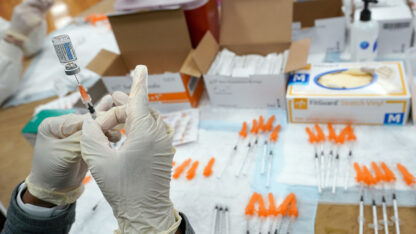
The Centers for Disease Control and Prevention is recommending updated COVID boosters, for people ages 12 and older.
These newly authorized shots are reformulated versions of the Moderna and Pfizer-BioNTech COVID-19 vaccines and they’re available at pharmacies, clinics and doctors’ offices around the country.
The boosters target both the original strain of the coronavirus and the two omicron subvariants which are causing most of the current infections. Vaccine makers have scrambled to rejigger the vaccines as they’ve become less effective against new variants.
Read this story now for free
To continue reading, sign up for our newsletter and get unlimited access to WABE.org
You can select your preferences for news and local content. We will never share your email address. Learn how your newsletter sign-up will support WABE and Public Media