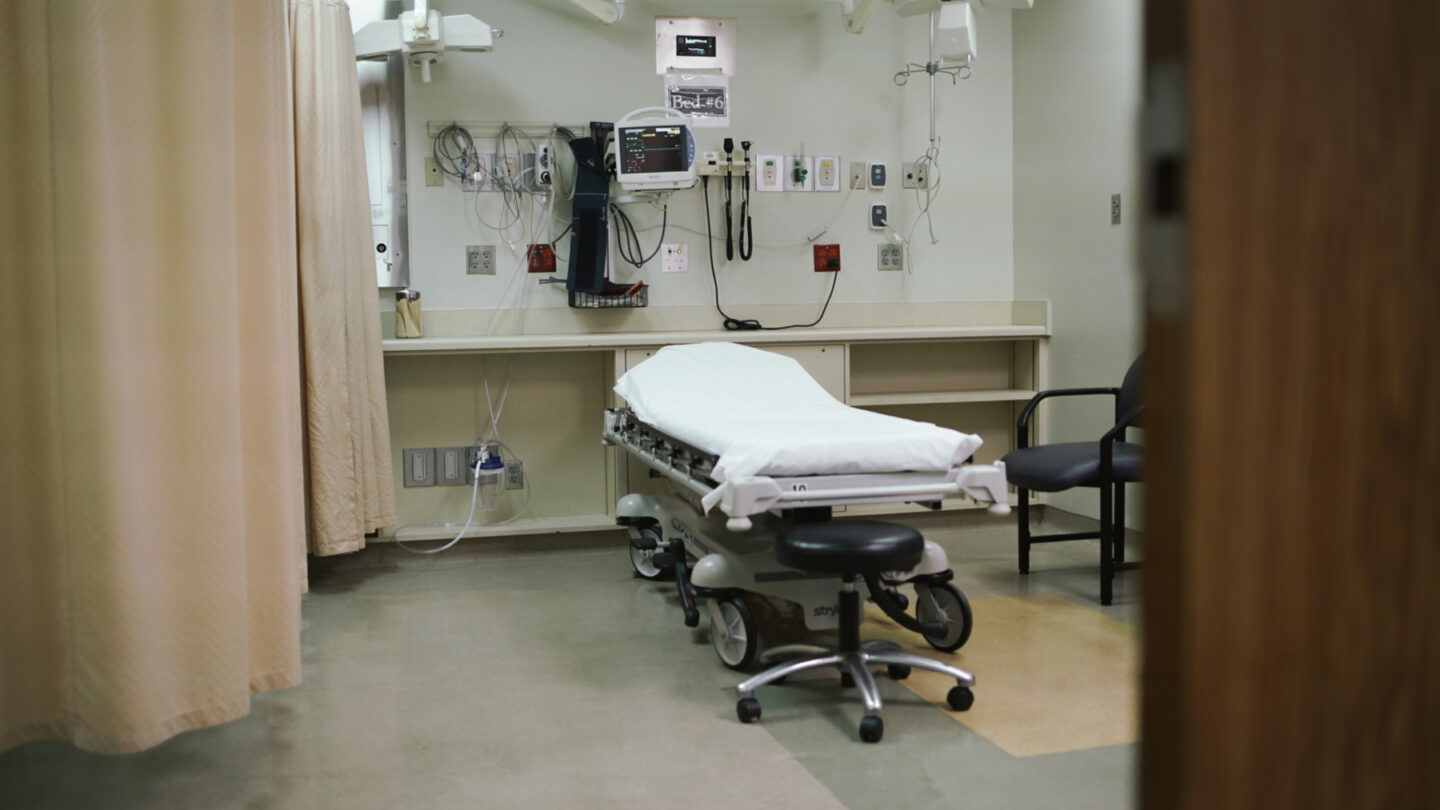
A lot of us have probably been to the hospital emergency room: For a broken bone, an asthma attack, the flu. Chances are, it wasn’t the best experience. Long wait times in crowded lobbies. Doctors hustling back and forth through the hallway. Cold, sterile rooms.
But that experience can be much worse if you step into the ER with a mental health emergency. And yet, Georgia’s emergency rooms are where patients often go during a mental health crisis – and at times, patients can be stuck there for days waiting for a space at a psychiatric facility to open up.
‘I got isolated in a room. It was scary.’
Ten years ago, Catherine Knight, a divorce attorney, was on her way to represent a client in court for an important trial. She was driving on Interstate 285 when suddenly she started to see and hear things she said she knew other people couldn’t see or hear. She pulled over to the side of the freeway.
Read this story now for free
To continue reading, sign up for our newsletter and get unlimited access to WABE.org
You can select your preferences for news and local content. We will never share your email address. Learn how your newsletter sign-up will support WABE and Public Media