Two months after the first monkeypox case was confirmed in Georgia, the state has emerged as a hotspot for the disease, with the fifth-highest number of infections in the nation.
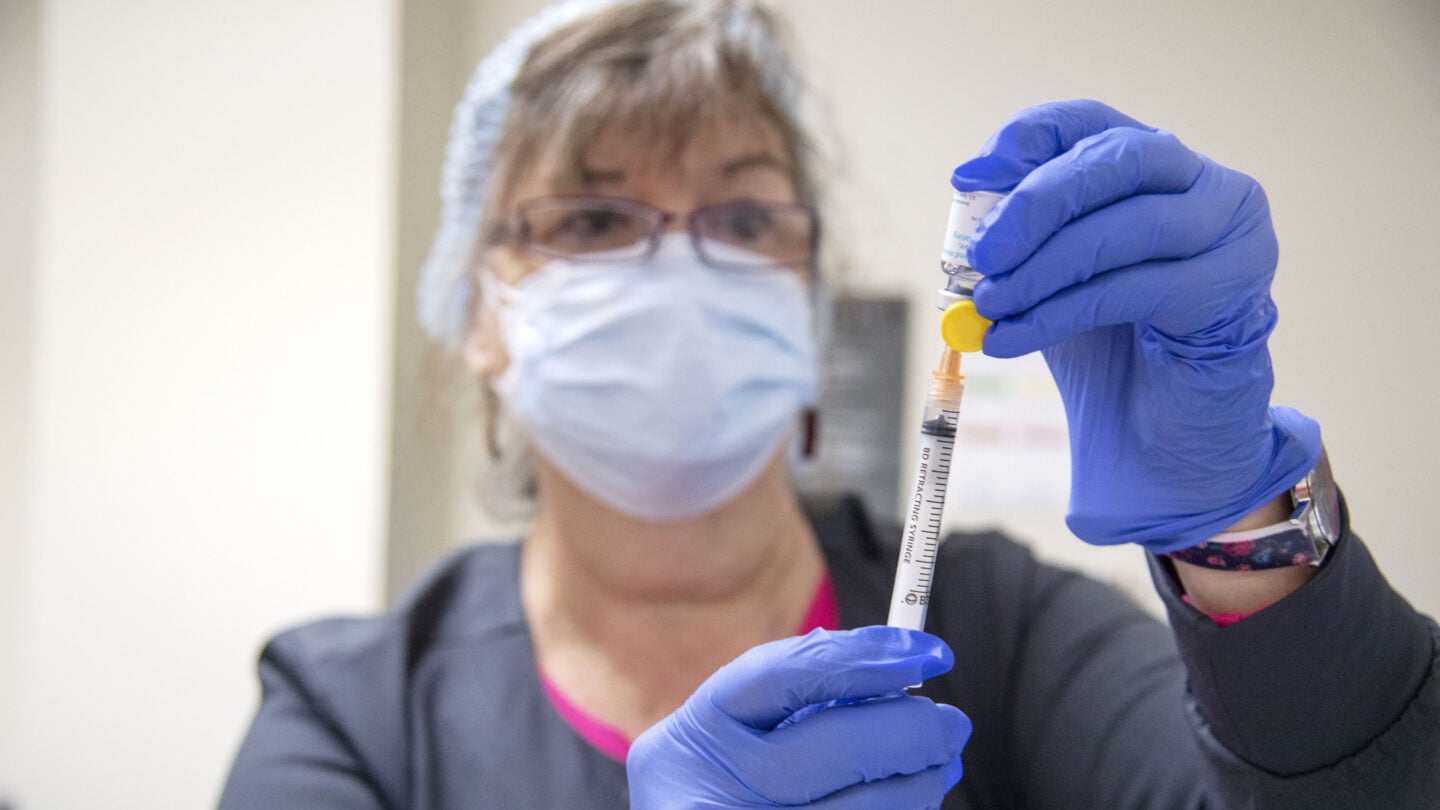
But a shortage in the number of vaccines available has led those most affected in the current outbreak — gay and bisexual men — to go on a frantic and often fruitless search for the shot. That combined with a lack of information about and availability of testing and treatment has brought up painful memories for a community scarred by past public health failures.
Gay Atlanta resident Ralph Mays started checking with local county health departments, health clinics and nonprofits for a monkeypox vaccine several weeks ago.
Read this story now for free
To continue reading, sign up for our newsletter and get unlimited access to WABE.org
You can select your preferences for news and local content. We will never share your email address. Learn how your newsletter sign-up will support WABE and Public Media